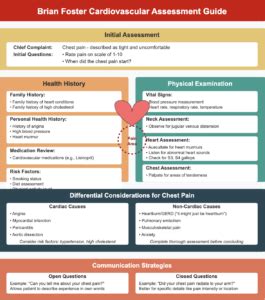
Understanding Brian Foster’s Cardiovascular Assessment in Shadow Health SBAR
In the healthcare field, timely and accurate communication is crucial for optimal patient outcomes. The SBAR protocol (Situation, Background, Assessment, Recommendation) is a powerful tool for this. When conducting a cardiovascular assessment on a patient like Brian Foster in Shadow Health, an understanding of SBAR becomes even more essential. Here’s a comprehensive guide to help you through the process with actionable advice, real-world examples, and a focus on solving common user pain points.
Problem-Solution Opening Addressing User Needs
Imagine you're a nurse or healthcare provider responsible for monitoring a patient like Brian Foster in a simulated environment. Understanding the nuances of cardiovascular health and effectively communicating your findings are vital. However, with a lot on your plate, ensuring you gather all necessary information and present it clearly using the SBAR method can be challenging. This guide is designed to provide step-by-step guidance with actionable advice to help you navigate these challenges, ensuring your communication is precise and patient outcomes are optimized.
Quick Reference
Quick Reference
- Immediate action item: Check Brian Foster's heart rate and blood pressure immediately upon contact.
- Essential tip: Use the SBAR format to concisely relay critical information to the healthcare team. Start with a clear situation statement, followed by background details, an assessment of the patient's condition, and end with a recommendation.
- Common mistake to avoid: Providing too much or too little detail in any section of the SBAR format. Aim for just enough detail to ensure your message is understood but avoid overwhelming the recipient with unnecessary information.
Detailed How-To Sections
How to Conduct the Situation
The Situation section of your SBAR communication should be brief and to the point. It serves as the opening hook that tells your healthcare team what the immediate problem is.
Here’s a step-by-step guide:
- State your name and position: “I’m Jane, a nurse in the cardiology unit.”
- Introduce the patient: “This is Brian Foster, a 56-year-old male with a history of hypertension and Type 2 diabetes.”
- Provide the current status: “His current heart rate is 120 bpm, and blood pressure is 160⁄95 mmHg.”
- Mention any urgent observations: “He reports chest pain rated 6⁄10 and shortness of breath.”
How to Craft the Background
The Background section provides context to support the situation. It includes the patient’s history, current medications, and any recent changes in their condition.
Here’s what to include:
- Briefly summarize Brian’s medical history: “Brian has a history of hypertension managed with lisinopril 10 mg daily and metformin 500 mg twice daily.”
- Note recent developments: “He was admitted yesterday with complaints of fatigue and elevated blood glucose levels.”
- Highlight relevant diagnostic results: “His latest ECG shows signs of early myocardial ischemia.”
How to Assess the Situation
The Assessment section involves interpreting the data you’ve gathered and explaining its significance to the patient’s current state.
Steps to follow:
- Summarize your findings: “Brian’s elevated heart rate and blood pressure, coupled with chest pain and shortness of breath, suggest a possible acute coronary syndrome (ACS).”
- Connect symptoms to likely conditions: “His symptoms align with those of ACS, potentially pointing to an impending myocardial infarction.”
How to Provide Recommendations
The Recommendation section is where you propose specific actions based on your assessment.
Key recommendations to consider:
- Request immediate cardiology consultation: “I recommend urgent cardiology assessment and possibly starting an IV nitroglycerin drip to manage his symptoms.”
- Advise on necessary tests: “I suggest running an urgent set of cardiac biomarkers and performing a repeat ECG.”
Practical FAQ
Common user question about practical application
One common question is: “What should I do if I’m unsure about my patient’s diagnosis in the SBAR format?”
Here’s a clear actionable answer:
When unsure about a diagnosis, focus on describing the current clinical picture without making definitive statements. Use language that reflects uncertainty such as “There are signs suggestive of,” or “The patient presents with symptoms consistent with.” This prevents overstating your conclusions and helps your team make informed decisions.
Best Practices and Tips
To ensure you are delivering effective and accurate SBAR communications, consider the following best practices:
- Be concise: Keep your SBAR communication succinct, focusing on the most critical details.
- Be clear: Use precise and clear language. Avoid medical jargon unless necessary and ensure it is explained.
- Use checklists: Create a checklist to ensure you cover all necessary components of the SBAR.
- Practice: Regularly practice using the SBAR format during simulations or drills to become more comfortable and proficient.
By following this guide, you will be better equipped to perform cardiovascular assessments on patients like Brian Foster in Shadow Health and communicate effectively using the SBAR protocol. This will not only improve your confidence but also contribute to better patient care through streamlined and precise communication.